Frequently Asked Questions












Getting Started
We work with young people ages 8-26 with serious mental health needs, such as depression, anxiety, bipolar disorder, trauma-related conditions, and conduct disorders. Many of our patients come to us after multiple hospitalizations, while on waitlists for residential treatment, or when weekly therapy alone hasn't been enough. If your kid needs more intensive support than outpatient care can provide, we might be a good fit.
Treatment is fully covered by insurance with no out-of-pocket costs for families. We handle all the billing directly with your health plan, so cost shouldn't be a barrier to getting your kid the care they need.
We're in-network with most major health plans, including Aetna, UnitedHealthcare, Anthem, Centene, and Amerihealth. Reach out and we can confirm in-network coverage.
Yes. We provide care in all 50 states through a combination of in-home visits and virtual sessions, so we can reach families wherever you are.
Treatment Approach
Your loved one works with a coordinated team of four professionals: a child and adolescent psychiatrist, a licensed therapist, a patient guide, and a family guide. These four care providers meet regularly to discuss your kid's progress and coordinate their approach, so you're not managing care alone anymore. Everyone stays on the same page about what's working and what needs to change.
Both. We combine in-home visits with virtual sessions to give your kid the best of both approaches. Our team comes to your home to build relationships and understand your environment, then stays connected through messaging and video sessions between visits. This hybrid approach means your kid can stay in school, keep their routines, and get care in the community where they feel most supported.
The full program is usually 52 weeks (one year) with multiple touchpoints every week. We adjust how often we check in based on what your kid needs: more support when things are hard, and we scale back as they stabilize. The year is broken into three phases: building stability (weeks 1-6), building skills (weeks 7-26), and building lasting change (weeks 27-52).
We use approaches proven to work for young people with serious mental health needs. The therapists draw from evidence-based methods like:
- Cognitive Behavioral Therapy -> helps young people change unhelpful thought patterns
- Dialectical Behavior Therapy -> teaches skills for managing intense emotions
- Acceptance and Commitment Therapy -> helps accept difficult feelings while taking action toward what matters to them
- Trauma-Informed Care -> recognizes how past experiences affect current behavior
We also work with you on parenting strategies that help lower the temperature at home and give you practical tools for tough moments. When appropriate, medication management is part of the plan too.
Here's what matters most: we know your family has probably tried other treatments before coming to us. Our approach is designed to meet you exactly where you are right now, whether your kid needs intensive support or is ready for less frequent check-ins. We adjust the level of care based on what your family needs, not a one-size-fits-all protocol.
Expect three or more contacts per week throughout the year. Your kid can text their patient guide between appointments to get support practicing skills in real life, not just during sessions. You can message or video call your family guide whenever you need help navigating tough situations at home.
Yes. Your family guide coordinates with your kid's existing doctors, school staff, and other providers. They share updates with your permission, can attend IEP meetings, and make sure everyone is working together. We work alongside your current support system, not instead of it.
In some cases, your kid may continue with an outside therapist or psychiatrist while also receiving care at Flourish. When this happens, we focus on clear communication and coordination so care isn’t duplicated and everyone understands their role, especially around medications and treatment goals.
Progress & Results
Most families see clinically significant improvement within 6 weeks: fewer crisis moments, better days at school, more connection at home. For young people with severe depression specifically, 54% improve in less than 4 weeks. Once things start improving, your kid may have some tough days, but they mostly keep getting better throughout treatment.
Every two weeks, we check in on how your kid is doing. Your care team uses their clinical expertise along with what you and your kid share with us. They also use validated assessment tools that measure specific symptoms. We use tools like PHQ-9 for depression, GAD-7 for anxiety, and CSSRS for safety concerns. This way we know what's actually helping based on data, not guesswork. If something isn't working, we adjust the approach right away.
An independent analysis by a major Medicaid health plan looked at our patients 6 months after they completed the program. Compared to similar kids who didn't receive Flourish Health care, our families had 70% fewer hospitalizations, 69% less residential treatment use, and 87% fewer partial hospitalizations. These results six months after program completion show that families learned skills that actually last.
Another health plan referred over 70 young people to us who were on waitlists for residential treatment. After working with Flourish Health, all of them improved and no longer needed residential care. They got the support they needed while staying home and going to school. For families, this meant their kids didn't have to leave home during a crisis. For the health plan, it represented a six-figure cost savings per patient, while delivering better outcomes.
Yes. We maintain 90%+ engagement every month across the full year, which is unusual for young people with serious mental health needs. We see 92% retention month over month, and 71% of caregivers are actively engaged every week. Staying connected is hard when life is chaotic, so we make it easier by providing technology, meeting you where you are, and taking some of the burden off overwhelmed parents.
The Clinical Team
Every person on your kid's care team completes extensive evidence-based training before working with families. They follow a shared Treatment Manual designed specifically for serious mental health needs. Your family gets consistent, high-quality care from providers who are prepared for what you're going through.
Flourish Health was founded by a Stanford-trained child and adolescent psychiatrist, and our clinical leaders come from places like Children's Hospital of Philadelphia, University of Virginia, Georgetown, and Mass General Brigham.
Yes. Every Flourish patient works directly with a child and adolescent psychiatrist. They are specialists with extra years of training specifically in treating young people. You get access to a psychiatrist without being stuck on a waitlist, which is rare in mental health care.
A licensed therapist provides evidence-based therapy tailored to your kid's specific needs, using proven approaches like Cognitive Behavioral Therapy, Dialectical Behavior Therapy, and trauma-informed care. They work closely with the other members of the care team to make sure everyone's approach is coordinated. The therapist focuses on teaching your kid skills to cope with overwhelming feelings and thoughts, while the patient guide helps them practice those skills in everyday life.
A patient guide checks in with your kid multiple times per week, helps with daily challenges, and serves as a consistent point of contact. They carefully build a trusting relationship with your kid and help them practice therapy skills in real-life situations, not just during scheduled appointments. Your kid can text them for support throughout the week.
Our Technology
Not a problem. We provide tablets and WiFi at no cost if technology is keeping your family from getting help. About 20% of our families use this benefit. Every patient has what they need to access care with Flourish Health.
Our care teams provide all patient care. AI tools never interact with patients or families directly. We use artificial intelligence and automation behind the scenes for administrative tasks, which frees up our clinicians to spend more time with patients instead of on paperwork. We're fully transparent about this and explain our use of AI tools as part of informed consent with every family.
Yes. All care is HIPAA-compliant, meaning your family's health information is protected and confidential. We use advanced encryption, conduct regular security audits, and have controlled access protocols. We only share information with your permission or when required by law to keep your child safe.
Yes, absolutely! Below are screenshots of our patient application and our staff application.
Patient application view:
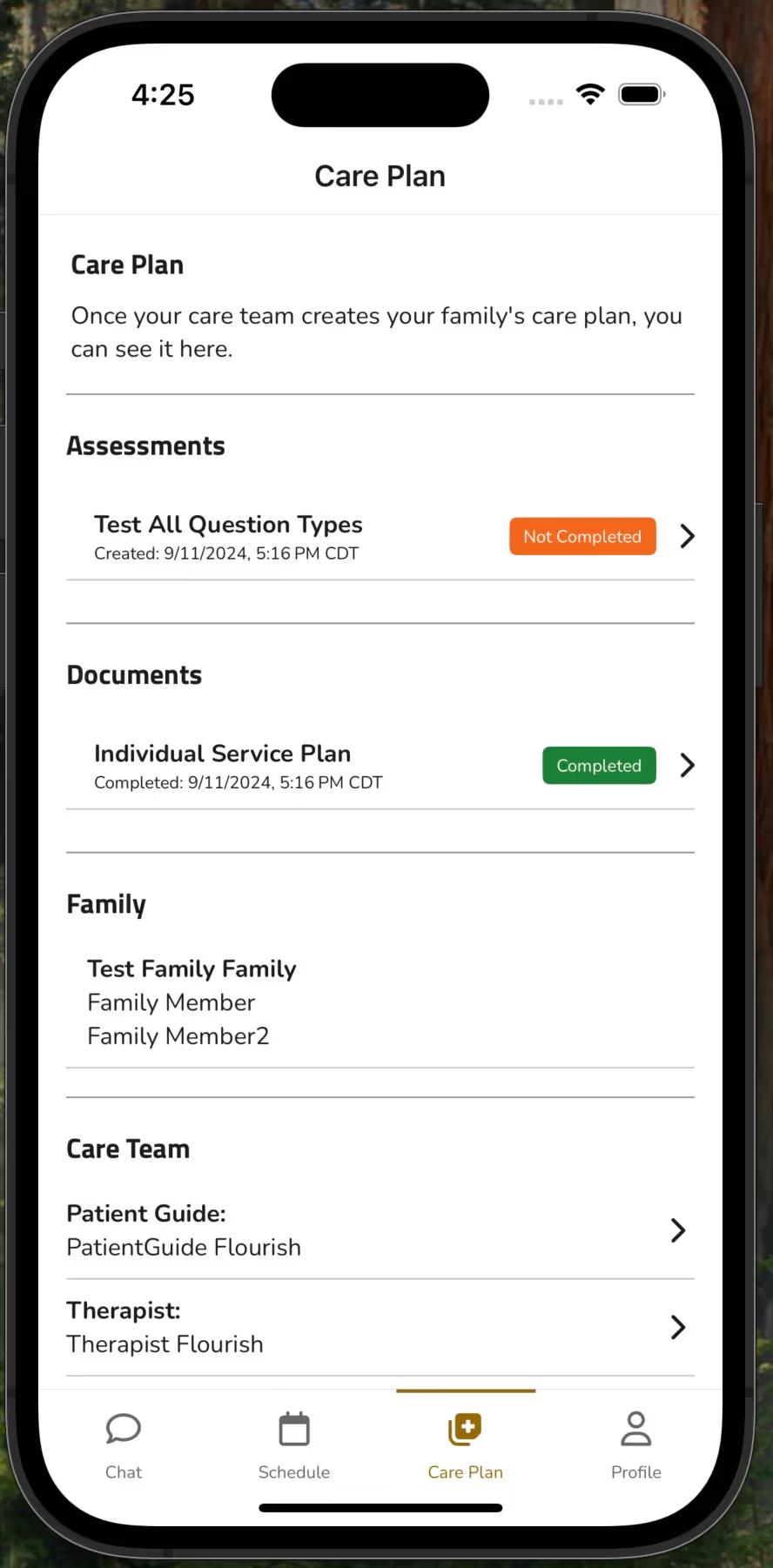
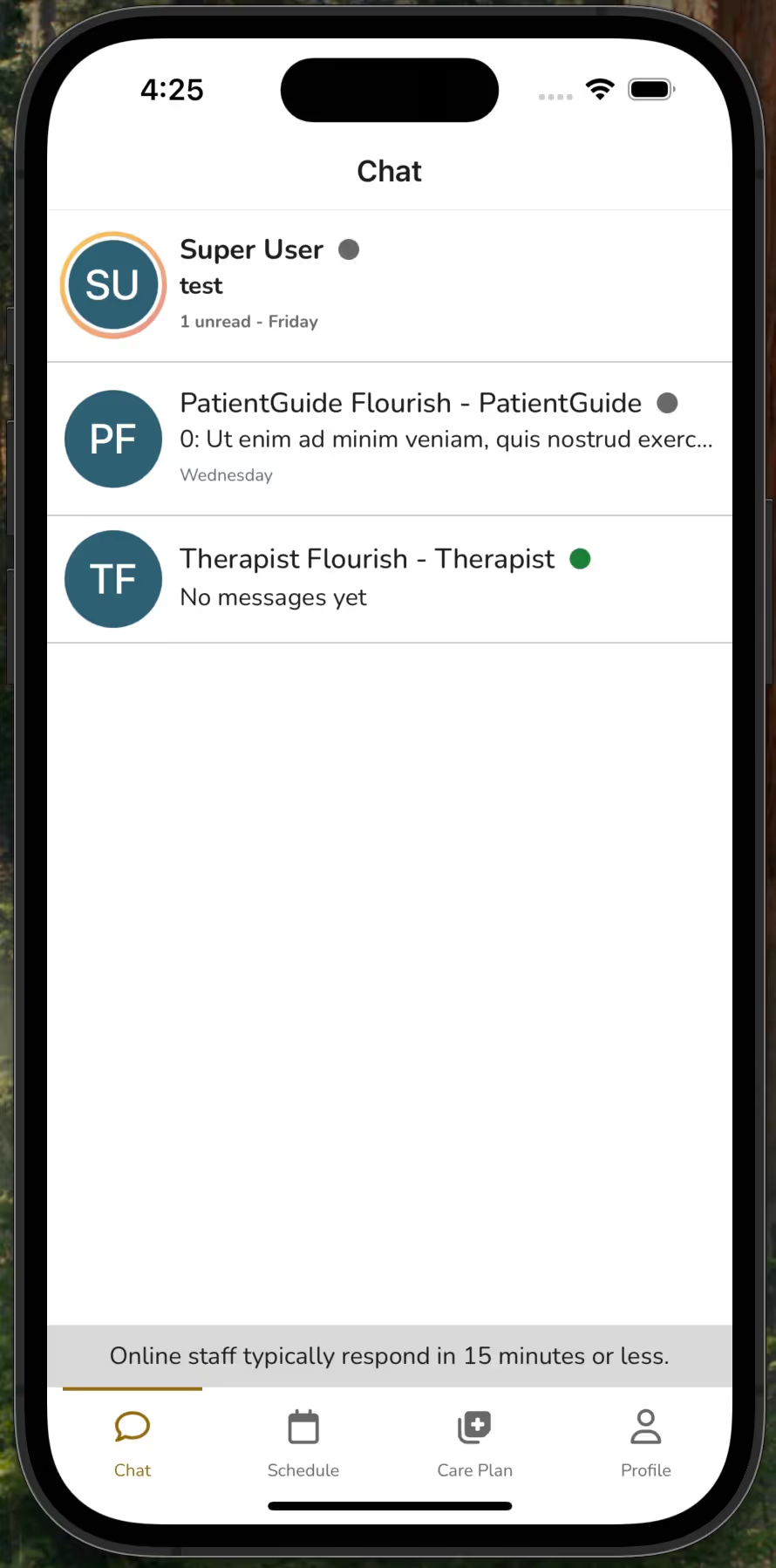
Staff application view:
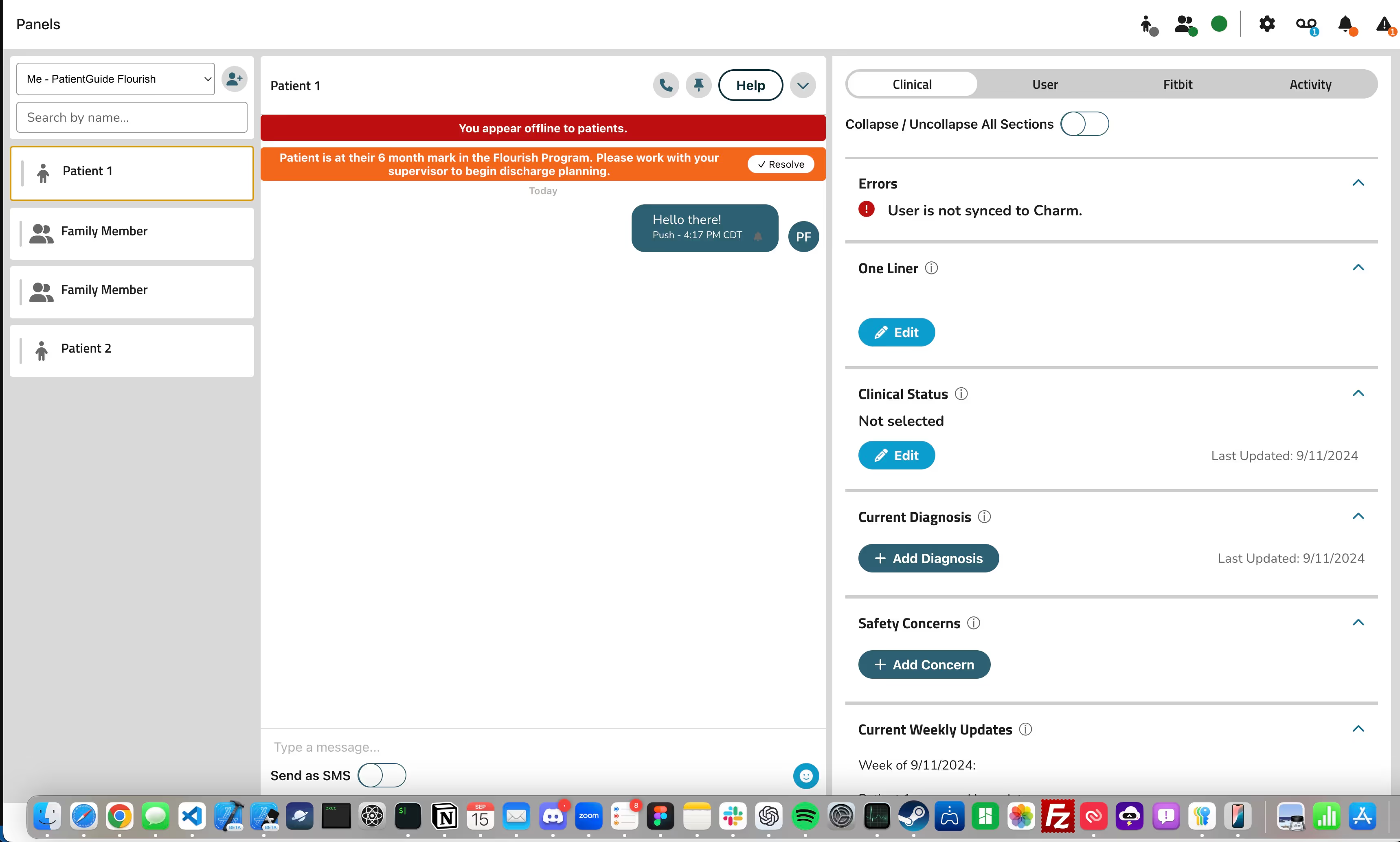
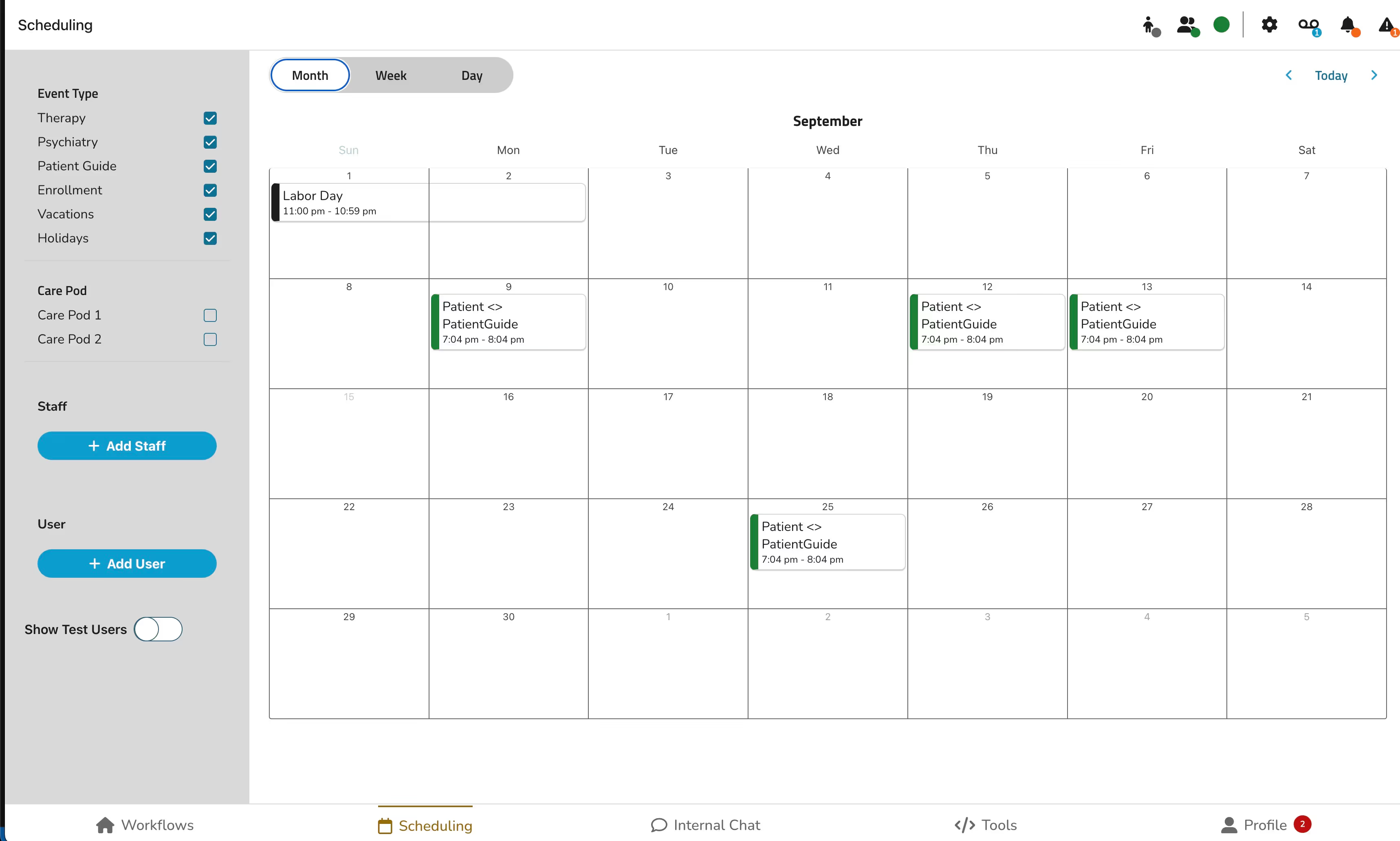
As a telehealth company, we use e-prescribing to ensure fast, accurate medication management for adolescents. It enhances safety by reducing errors, checking for drug interactions, and providing instant access to prescriptions. E-prescribing also supports treatment compliance and integrates seamlessly with our virtual care plans for comprehensive mental health support.
No, but we can send prescriptions to any pharmacy we support.
Our workflow ensures that the prescriber retains full discretion in choosing the most suitable medication based on the patient’s needs and clinical judgment. At the same time, the patient is given the flexibility to select the pharmacy of their choice for filling the prescription. This approach allows for personalized, patient-centered care, ensuring that both the medication and the pharmacy align with the patient’s preferences and convenience, while maintaining the highest standards of clinical care.



